If your child has sustained playground injuries, you may have grounds to file a claim or lawsuit seeking compensation.
Financial compensation may be available when a child is injured while playing on a backyard trampoline.
Taking the right steps after a child’s bicycle accident can help them recover while boosting your odds of securing compensation.
Financial compensation may be available when a child is injured while playing on a backyard trampoline.
Taking the right steps after a child’s bicycle accident can help them recover while boosting your odds of securing compensation.
Compensation may be available for your injuries and related losses if you were hurt in a boating accident resulting from negligence.
If your child has been harmed in a drowning accident resulting from another’s negligence, compensation may be available.
Financial compensation may be available if your child is injured during a school field trip, even if you signed a liability waiver.
Yesterday afternoon in the northern section of the state, namely the Lawrence / Andover / Merrimack Valley area, there were
Compensation may be available when a child is injured because of a defective car seat in Massachusetts.
Safety of children should be the primary concern of every parent when buying toys. World Against Toys Causing Harm, Inc,
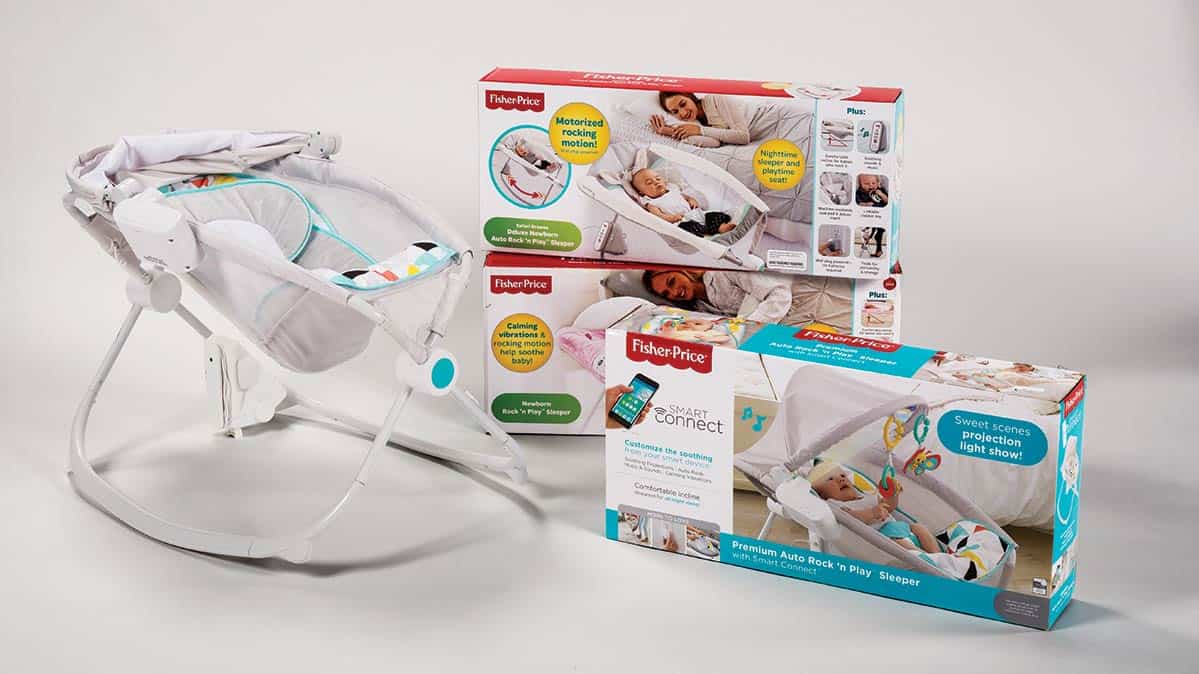
SOURCE: Consumer Product Safety Commission Fisher-Price and the Consumer Product Safety Commission today issued a product warning